Results
Remote Consults A Year
“We were looking for a solution that worked in a challenging technology landscape; where there’s a mix of satellite connectivity, high bandwidth, low bandwidth, high latency, as well as terrestrial infrastructure”
Key Results
The Alaska Native Tribal Health Consortium (ANTHC) was established in 1997 to manage statewide health services for Alaska Native and American Indian people. Because of the obvious need for a statewide telehealth solution to supplement tertiary healthcare, in 1998, ANTHC implemented a statewide telehealth program (AFHCAN) that was initially built using “store and forward” technology. AFHCAN is a multifunctional telehealth solution that combines hardware and software components designed to facilitate communication between providers, allowing them to capture and share data. However, until recently, what was missing from this system was live audio and video capabilities. According to Stewart Ferguson, ANTHC CIO, “As we branched out into more and more telehealth, we recognized that not having the video and audio components was a barrier to expanding our capabilities to better serve our communities.”
ANTHC estimates that it costs about $300 in travel to transport a patient from a village to one of its regional facilities, and $900 to get them to the hospital in Anchorage. When a family member travels with the patient, it’s double that amount. The need for a solution that enhanced AFHCAN’s existing system with affordable, high-quality video and audio became more and more evident. Ferguson estimates that, typically, two thousand dollars per patient is saved in travel costs when telemedicine is used; twenty thousand dollars or more when the need for emergency medical evacuation is eliminated using telemedicine.
“Vidyo is great,” said Ferguson. “We were looking for a solution that worked in a challenging technology landscape; where there’s a mix of satellite connectivity, high bandwidth, low bandwidth, high latency, as well as terrestrial infrastructure. We also needed a solution that was simple. There’s no real opportunity to train the people who use our system. We have about 1.5 thousand providers in our network. On average, 500 new providers join each year. That’s a challenge because these providers are out in the remote areas of the state, not in Anchorage. They need to be able to easily access and use Vidyo without training so the solution had to work reliably and provide the highest quality video, audio and data sharing that we could find. Vidyo excels on all of these fronts.”
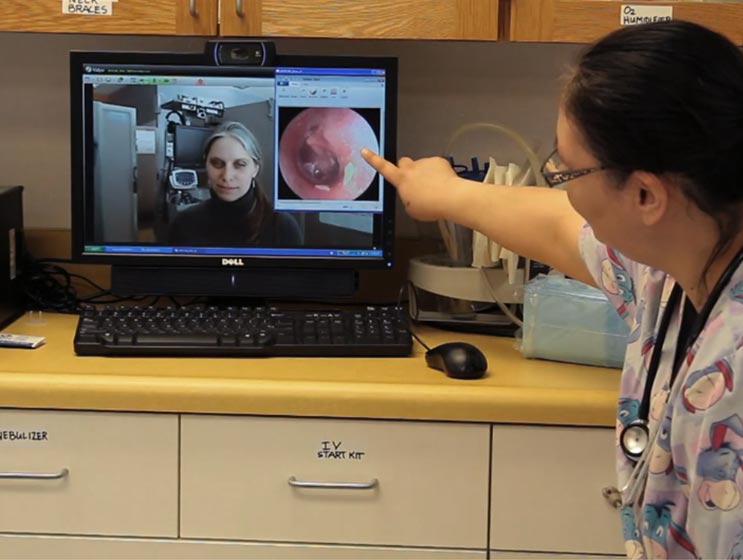
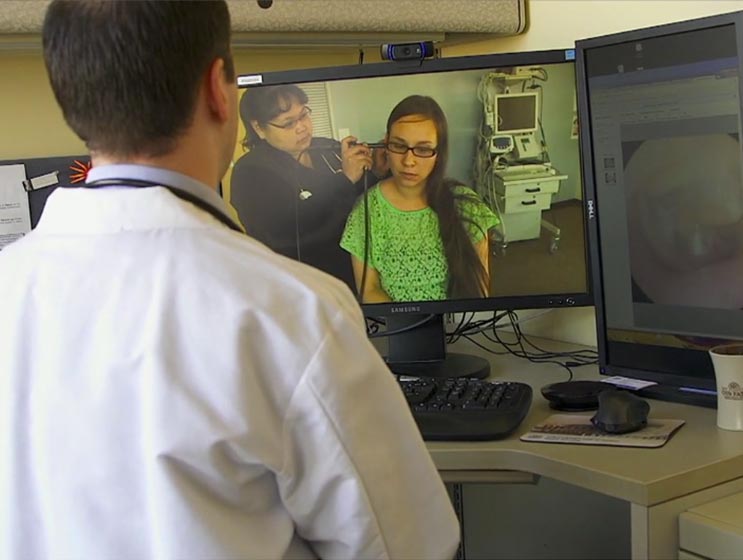
Dr. Ella Derbyshire, Medical Director of the Maniilaq Health Center in Kotzebue, Alaska, attests to how much Vidyo has expanded and strengthened what health practitioners are now able to accomplish: “I’m in Kotzebue and my patients are in in Selawik, which is about 90 miles away. With telemedicine I can look inside of a child’s ear to see if they have an infection, I can oversee a resuscitation procedure or the birth of a baby via Vidyo. It’s a very important element to providing quality medical care here. Before telemedicine, if we had an emergency in the village — let’s say a snow machine crash — we would not be able to adequately assess the patient’s condition. We would have to rely on a community health aid practitioner to describe the patient’s condition to determine if this is someone who needs to come into Kotzebue … or can stay where they are … or needs to be transported by plane directly to the medical center in Anchorage if they’re so acute that they need to see a surgeon immediately.”
“The nice things about building our solution around Vidyo is that we can also expand into other areas that we haven’t been able to support such as statewide behavioral health, suicide prevention, and supporting sexual abuse response teams,” said Ferguson. “There are so many things we can offer when we have such a reliable technology. Our providers, interestingly enough, are driving this. Typically in a telehealth program, you have to urge providers to get involved. But we’re now at a point with critical mass where it’s actually our providers from a variety of areas – cardiology, pulmonology, tele-trauma, tele-ICU, tele-stroke– who are demanding solutions based on live video. Practically every provider that comes to our campus now is asking us what they can do to provide care over live video to our villages and our remote regions.”
Dr. Derbyshire explains that “over Vidyo you are able to make eye contact with the patient so they can see that you’re giving them 100% of your attention and they are actually relating to you via that eye contact. You ask them a question and they respond immediately. You can ask them to ‘show me where it hurts’ and you can see where they’re pointing to, you can discern if they are in pain or if they don’t seem all that uncomfortable. You really make a connection and have a better feel for what’s going on and the patient seems to understand that. It’s so much better than communicating over telephone or email … it’s real, it’s personal and it’s immediate.”
ANTHC currently oversees over 40,000 consults a year statewide, but looking into the future, Ferguson predicts that Vidyo makes it possible for practitioners to reach many more patients. “We have providers who want to reach out to their patients and to their colleagues, independent of location. My vision for the future of this is that, as we discharge patients from the hospital, there will be a standing order under certain circumstances to do telehealth follow ups where practitioners connect with patients in their homes and perhaps use remote technology to monitor a patient’s recovery, depending on what the situation calls for. Distances will disappear, and what happens in that kind of a mix is that healthcare practitioners who are sharing data and communicating are able to provide better treatment.”
Dr. Derbyshire concurs and offers one further significant observation: “When we have to take a patient out of their village to bring them to the clinic in Kotzebue, we are taking them away from their support system. The people who help them deal with their injuries or illnesses are left behind. It really is important that we provide a continuity of care. If we can keep them in their village and provide quality healthcare via Vidyo-enabled telemedicine right where they live, I believe that we will have much better outcomes.”

Get In Touch With Sales
Learn more about how Vidyo can provide the solution you need.
